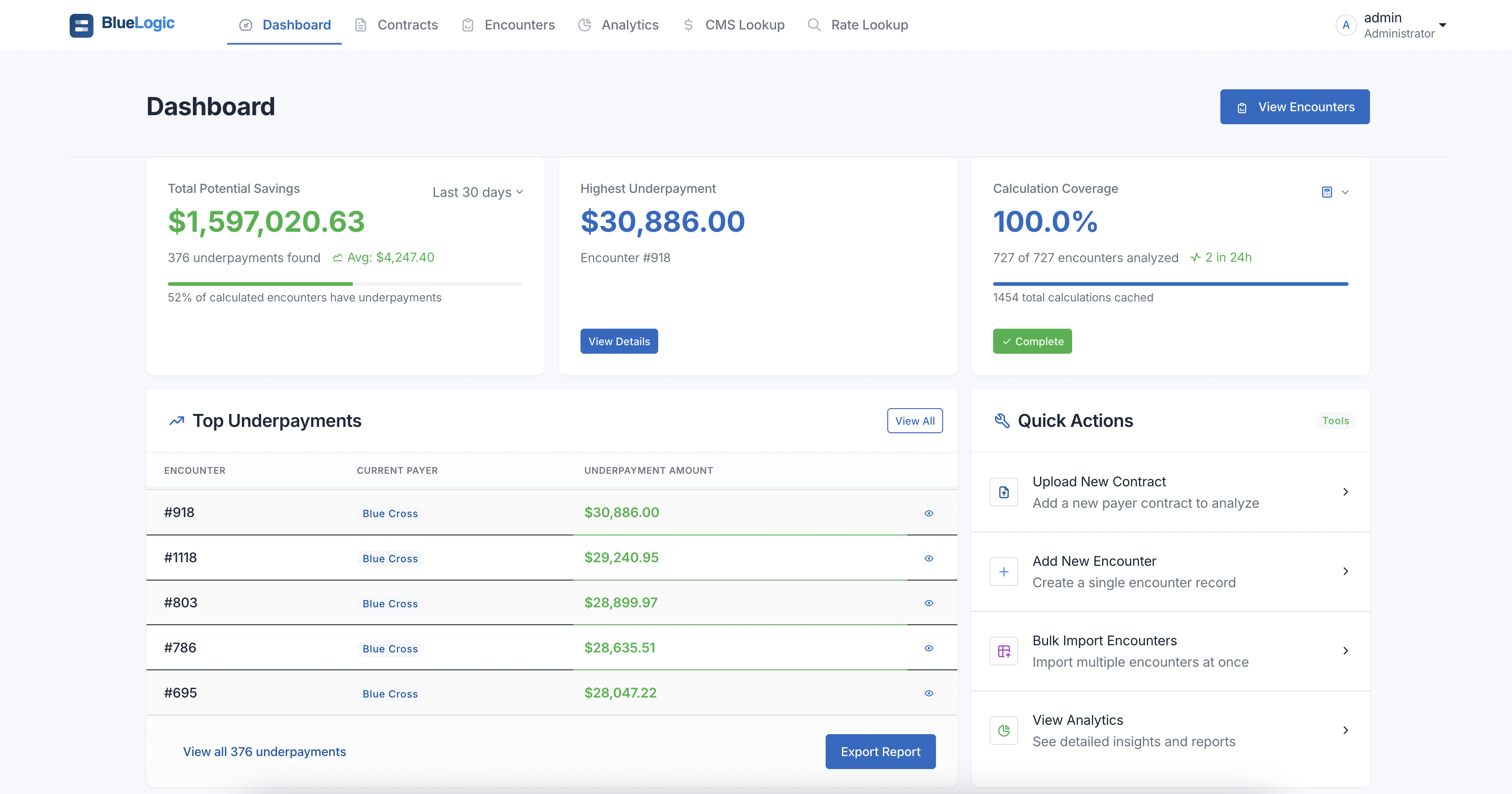
Intelligent Healthcare Contract Analysis
BlueLogic™ is a healthcare revenue recovery consultancy that identifies and recovers underpayments through AI-powered contract analysis, helping hospitals maximize their legitimate reimbursement.
Already built machine-readable files for price transparency? Use that rate data to detect underpayments instead of treating compliance work as a sunk cost.
Patent Pending
Healthcare providers average $2 million in reclaimed revenue annually